Since the start of the COVID-19 pandemic, we’ve stayed home more, often delaying medical care. Of course, this means delaying procedures that are purely optional. But if you’ve developed a leg ulcer, your treatment and follow-up care isn’t optional. In fact, it’s crucial to your health—especially in terms of preventing amputations!
Under the circumstances, we’d like to share a suggested screening protocol for your vein specialist visit. Keep in mind, every office visit will be different. But if you’ve had or are currently dealing with a leg ulcer, consider this your assessment guidelines. 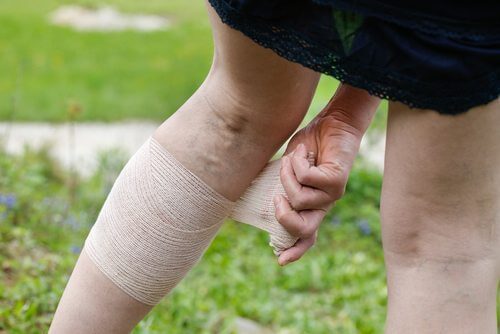
Leg ulcers are just open sores that don’t heal in the typical time-frame. Often, you develop leg ulcers if you have chronic vein problems. Typically, they develop around your ankle, ranging in size from very small to several inches in diameter. Sometimes, these sores don’t hurt that much. But, for many patients, their venous ulcers become very painful and develop infections.
Why does chronic vein disease lead to ulcer development? CVD causes inflammation in your body, and that inflammation damages your capillaries and lymphatic ducts. This damage allows fluid to leak out of your capillaries, which can cause swelling in your lower legs. And, as fluid builds up in your leg’s soft tissue, sores may develop.
So, now you’ve got a sore. But why won’t it heal? Here’s the story: that capillary damage also means your lower legs have lower oxygen levels. And less oxygen inhibits your body’s ability to heal itself. That’s when your open sores or ulcers stick around. Unless, of course, you seek treatment.
When you come into our Houston and Dallas area vein clinics, we’re going to address your ulcer. But we’ll also treat your underlying condition, so you don’t keep dealing with these open sores.
In order to treat your ulcer, we’ll take a two-pronged approach: wound care and compression therapy. We’ll care for your wound by keeping the sore clean to prevent infection. And we’ll dress it with sterile bandages to keep your wound clean.
We’ll also recommend appropriate compression therapy, in the form of prescription level compression stockings. These stockings will increase blood flow to your lower legs, which will help speed up your healing process.
Studies now suggest that a drug called Oxybryta could play an important role in leg ulcer care if you have sickle cell anemia. While anyone with vein issues may develop leg ulcers, between 14% and 18% of people with sickle cell will get one.
Right now, this drug is only approved for treating leg ulcers in people with sickle cell disease who are over the age of 12. Still, it's promising news for anyone with compromised circulation or a risk for leg ulcers. And we'll carefully watch this and other developments to help offer the best leg ulcer care to our patients.
Once your wound is on the path to healing, we can address your underlying vein condition. To do so, we’ll close up the vein that isn’t working properly. Once closed off, blood will flow through the veins that are working appropriately, helping return optimal oxygen levels to your lower legs, and preventing further complications.
We know these are scary times, but leg ulcers are also scary medical developments. So we don’t want you to compromise your vein or limb health out of fear. Please know that we are taking every precaution in our office to protect you and our team members. So don't wait another day to address your vein health. Make an appointment todayMake an appointment todayMake an appointment today to address your ulcers and underlying conditions.
Sources: American Journal of Hematology, Healthcare Improvement Scotland,

Scheduling
Please contact our dedicated specialists to schedule a consultation today.
2024 Texas Endovascular. All rights reserved. Website Design by Healthcare Success